The VA Claim Pre-Filing Checklist: What Your Claim Actually Needs Before You Submit

- 1.The Problem With Generic VA Claim Checklists
- 2.Start Here: The Three Elements of Service Connection
- 3.Know Your Claim Type - It Determines What Evidence You Need
- 4.The Pre-Filing Checklist
- 5.Phase 2 Claim-Type Specific Evidence
- 6.Phase 3 Optional - But Can Strengthen Your Claim.
- 7.What You Don't Need to Upload
- 8.Frequently Asked Questions
- 9.Not Sure Your Claim Is Ready?
The Problem With Generic VA Claim Checklists
Search "VA claim checklist" and you'll find dozens of lists telling every veteran to gather the same stack of documents: upload your DD-214, get a nexus letter, complete a DBQ, pull your service treatment records. As if every claim is identical.
They're not. And treating them that way is one of the reasons veterans either file with evidence they don't need - or worse, skip evidence they do.
Here's the reality: the VA already has your DD-214 and service treatment records in their system. You don't need to upload them. What you do need depends on what type of claim you're filing - direct, secondary, presumptive, or aggravation - because each pathway has different evidence requirements under 38 CFR.
This pre-filing checklist is structured around that principle. It starts with what every veteran needs regardless of claim type, then shows you what additional evidence your specific pathway requires. It also tells you what you don't need - because filing smarter means focusing on what's necessary, not what's billable.
Our Approach:
Not every claim needs a nexus letter. Not every claim needs a private DBQ. We'll tell you that honestly - because the goal is to help you file a claim that's ready, not to sell you services you don't need. That's the foundation of every Claim Readiness Review we conduct.
Start Here: The Three Elements of Service Connection
Before anything else, understand the foundation. Under 38 CFR § 3.303, every VA disability claim requires three elements for service connection to be granted. If any one is missing, the claim will likely be denied — regardless of how legitimate your condition is.
Element 1: A current medical diagnosis. Not symptoms. Not a self-assessment. A formal diagnosis from a qualified medical provider, documented in your medical records.
Element 2: A basis for service connection. This is where claim type matters. For a direct claim, it's an in-service event, injury, or exposure. For a secondary claim, it's an already service-connected condition. For a presumptive claim, it's qualifying service that meets the presumptive criteria.
Element 3: A medical link (nexus) between Element 1 and Element 2. This is the connection. For some claim types, the VA presumes this link. For others, you need to demonstrate it — and that's where evidence like a nexus letter comes in.
38 CFR § 3.303(a): Service connection requires evidence of a current disability, an in-service incurrence or aggravation of a disease or injury, and a medical nexus between the claimed in-service event and the present disability.
Know Your Claim Type - It Determines What Evidence You Need
This is the step most generic checklists skip, and it's the most important one. Your claim type dictates which evidence is required, which is helpful but optional, and which is unnecessary. Here's how the four main pathways differ:
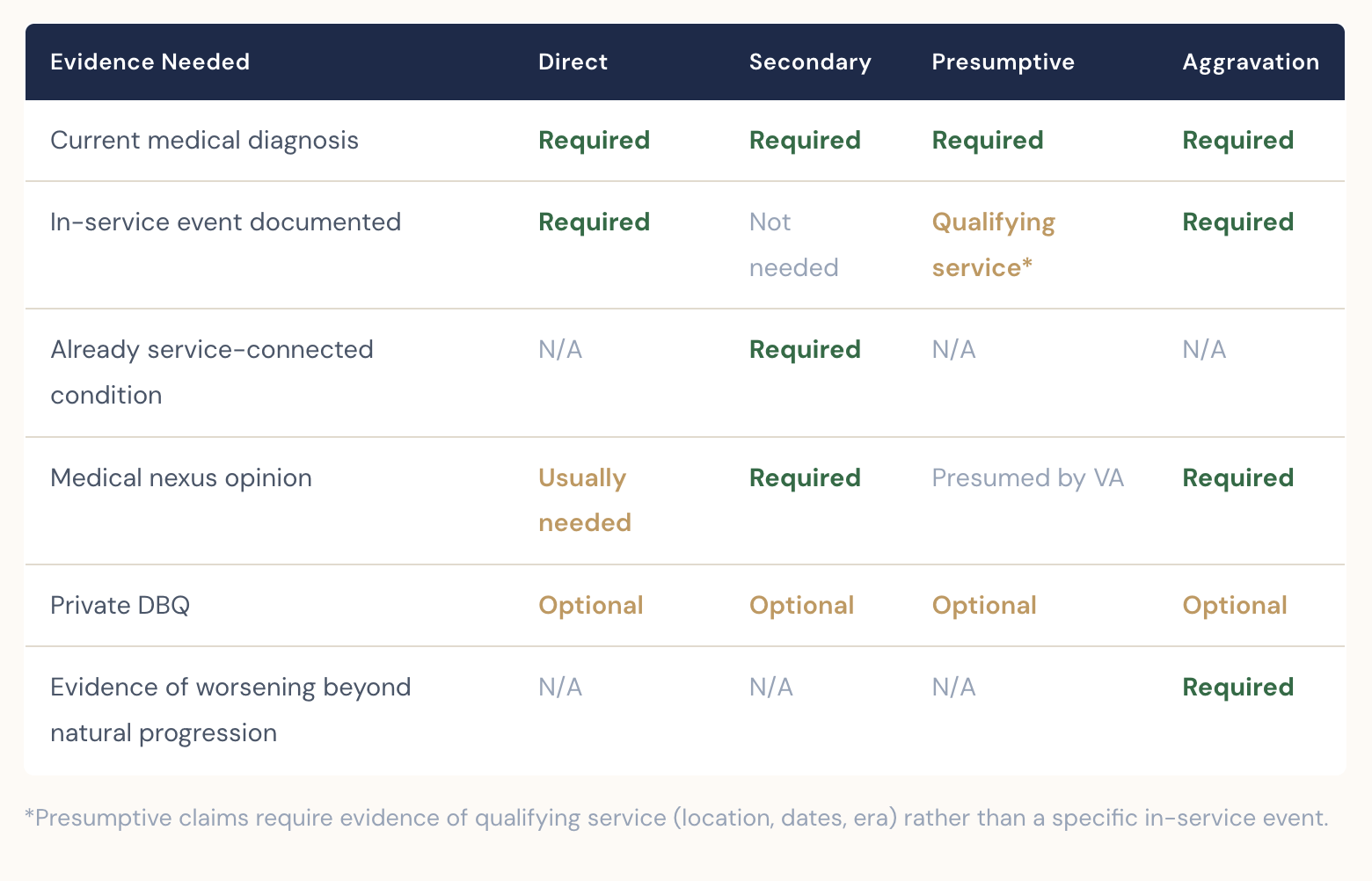
The Pre-Filing Checklist
Phase 1 Every Claim — Regardless of Type
#01Intent to File Is Submitted (VA Form 21-0966)
Before you build your evidence package, protect your effective date. An Intent to File tells the VA you plan to submit a claim and gives you one year to complete it. If your claim is approved, the VA can backdate benefits to the ITF date. Skip this step and your effective date defaults to the day the VA receives the completed claim - potentially costing you thousands in retroactive pay.
Applies to: All claim types.
#02Identify Your Claim Type
This determines everything that follows. Are you filing a direct claim (condition caused by an in-service event)? A secondary claim (new condition caused or aggravated by an already service-connected condition)? A presumptive claim (condition on a VA presumptive list for your era/location of service)? Or an aggravation claim (pre-existing condition that worsened beyond natural progression during service)? If you're not sure, that's exactly what a Claim Readiness Review helps clarify.
Applies to: All claim types.
#03Confirm You Have a Current, Documented Diagnosis
The VA cannot grant service connection without a current diagnosis from a qualified medical provider recorded in your medical records. "My back hurts" documented in treatment notes is not the same as "lumbar degenerative disc disease" with an ICD-10 code. If you have symptoms but no formal diagnosis, schedule an evaluation before filing. This is the foundation of every successful claim.
Applies to: All claim types.
#04Review Your Post-Service Treatment Records
The VA needs to see what's happening with your condition now. Make sure your recent treatment records — VA, private, or both — document your current symptoms, treatment, and functional limitations. If you haven't been seen for a condition in over a year, a rater may question whether it still meets rating criteria. You don't need to upload VA records (the VA has them), but private treatment records should be submitted or authorized for release.
Applies to: All claim types.
#05Write a Personal Impact Statement
In your own words, describe how your condition affects daily life, work, and relationships. Be specific about functional limitations, not just pain. Instead of "my knee hurts," write: "I can no longer climb stairs without holding the railing. I had to stop running. I wake up 2-3 times per night from pain and stiffness." Raters use this to understand the real-world impact that clinical records may not capture.
Applies to: All claim types (Strongly Recommended).
Phase 2 Claim-Type Specific Evidence
This is where the evidence requirements diverge. Complete only the items that apply to your claim type.
If You're Filing a Direct Claim
#06aIn-Service Event, Injury, or Exposure Is Documented
Your evidence must establish that something happened during service — an injury, illness, toxic exposure, or traumatic event. This might already appear in your service treatment records (which the VA has), but supporting evidence like deployment records, MOS documentation, incident reports, or combat records can strengthen it. If your STRs don't document the event, buddy statements and lay evidence become critical.
Applies to: Direct and/or TERA Claim.
#07ADo You Need a Nexus Opinion?
If the connection between your in-service event and your current diagnosis is straightforward and well-documented in your records, a C&P exam may be sufficient to establish the link. But if there's a gap in documentation, the connection isn't medically obvious, or you want to ensure a qualified clinician reviews your full history before the VA makes a decision — a nexus letter stating the condition is "at least as likely as not" connected to service can be the deciding factor.
Applies to: Direct and/or TERA Claim (Case by Case).
If You're Filing a Secondary Claim
#06bYour Primary Condition Is Already Service-Connected
A secondary claim connects a new condition to one the VA has already recognized as service-connected. Confirm the primary condition's service connection is active in your VA records. Common secondary pathways include PTSD leading to sleep apnea, a knee injury altering gait and causing hip or back pain, or medication side effects causing a new diagnosis.
Applies to: Secondary Claim.
#07bMedical Nexus Linking the New Condition to the Service-Connected Condition
For secondary claims, the nexus opinion is almost always essential. It must explain the medical mechanism by which the already service-connected condition caused or aggravated the new condition. Under 38 CFR § 3.310, the VA requires evidence showing the new disability is "proximately due to or the result of" the service-connected condition. A qualified clinician with expertise in the relevant specialty should author this opinion with supporting medical rationale.
Applies to: Secondary Claim.
38 CFR § 3.310: Disability which is proximately due to or the result of a service-connected disease or injury shall be service connected. When aggravation of a nonservice-connected condition is proximately due to a service-connected condition, the veteran shall be compensated for the degree of disability over and above the degree existing prior to the aggravation.
If You're Filing a Presumptive Claim
#06cYour Service and Diagnosis Match a Presumptive List
Presumptive conditions — including those under the PACT Act for burn pit and toxic exposure, Agent Orange, Gulf War illness, and radiation — do not always require a nexus letter. The VA presumes the connection. What you need is evidence that you served in the qualifying location/era and that you have a diagnosed condition on the presumptive list. Your service records (which the VA has) typically establish the qualifying service; your medical records establish the diagnosis.
Applies to: Presumptive Claim.
If You're Filing a Aggravation Claim
#07bEvidence the Condition Worsened Beyond Natural Progression During Service.
If you entered service with a pre-existing condition and it worsened, you may qualify for service connection through aggravation. The key is showing that the worsening went beyond natural progression — meaning service made it worse than it would have gotten on its own. This typically requires a medical opinion addressing the baseline severity at entry, the severity at separation, and why the increase is attributable to service rather than the natural course of the condition.
Applies to: Aggravation/TERA Claim.
Phase 3 Optional - But Can Strengthen Your Claim.
#08Buddy Statements or Lay Evidence (VA Form 21-10210).
Written statements from fellow service members, family, or coworkers are admissible evidence. A buddy who witnessed your injury, a spouse who describes how PTSD affects daily life, or a coworker who notes your functional limitations - all of these add context that clinical records alone may not capture. Not every claim needs them, but they can fill documentation gaps, especially when STRs are incomplete.
Helpful for: Claims with documentation gaps, PTSD Stressor corroboration.
#09Private DBQ (Disability Benefits Questionnaire).
A private DBQ is not required. The VA will schedule a C&P exam where an examiner completes the relevant DBQ. However, a privately completed DBQ from a clinician who knows your full history can ensure your symptoms and functional limitations are thoroughly documented especially if you're concerned a brief C&P exam won't capture the complete picture. Each condition has a specific DBQ with measurements that map directly to rating criteria in 38 CFR Part 4.
Optional for: All claim type - consider when thorough documentation matters.
#10Claim Filing Strategy: FDC vs. Standard, Condition Priority.
A Fully Developed Claim (FDC) tells the VA all evidence is submitted and ready - it typically processes faster. But only choose FDC if your evidence is genuinely complete. If you're still waiting on records or opinions, file a Standard Claim instead. Also consider whether filing all conditions at once is the best approach, or whether focusing on your strongest, highest-impact conditions first will produce a better outcome.
Strategic Decision: All claim types.
What You Don't Need to Upload
Common misconception: Many checklists tell you to upload your DD-214 and service treatment records (STRs) with your claim. You don't need to. The VA already has your DD-214, personnel file, and STRs in their system from your military service. You should have your own copies for reference when building your case so you can identify relevant STR entries, confirm deployment dates, or prepare for a C&P exam - but you don't need to submit them as part of your claim package.
Frequently Asked Questions
Do I need a nexus letter to file a VA disability claim?
Not always. Presumptive conditions — such as those covered under the PACT Act — generally do not require a nexus letter because the VA presumes the service connection. Direct claims with clear in-service documentation and an obvious medical link may also succeed without one. However, for secondary claims, claims with documentation gaps, or any claim where the medical link isn't self-evident, a nexus letter from a qualified clinician can be the deciding factor. A Claim Readiness Review can help you determine whether your specific claim needs one.
What's the difference between a direct, secondary, and presumptive VA claim?
A direct claim connects a condition to a specific in-service event, injury, or exposure. A secondary claim connects a new condition to an already service-connected disability - for example, sleep apnea caused by service-connected PTSD. A presumptive claim applies when the VA automatically presumes service connection because you served in a qualifying location or era and have a condition on the presumptive list. Each pathway requires different evidence — the matrix above breaks it down..
What is the most common reason VA claims get denied?
The most frequent reason is a missing or inadequate nexus — the medical link between a diagnosis and service. Other common denial reasons include having no current diagnosis on record, insufficient evidence of severity or functional impact, and not attending a scheduled C&P exam. Understanding why claims get denied is the first step to building one that doesn't.
Do I need a private DBQ before filing?
No. The VA will schedule a C&P exam where the examiner completes the relevant DBQ. A private DBQ is optional but can help ensure thorough documentation of your symptoms and limitations — especially for conditions where a brief exam might not capture the full picture. It's a tool to strengthen your claim, not a prerequisite to file one.
How do I know if my VA claim is ready to file?
Your claim is ready when you can confirm three things with evidence: (1) a current documented diagnosis, (2) an identified basis for service connection appropriate to your claim type, and (3) a medical nexus establishing the link — if your claim type requires one. If you're unsure about any of these elements, our free claim readiness diagnostic can give you a quick assessment in two minutes.
Not Sure Your Claim Is Ready?
A Claim Readiness Review identifies exactly what's in your file, what's missing, and whether you actually need a nexus letter, a DBQ, or nothing at all.
We focus on what's necessary — not what's billable.
Request a Claim Readiness Review — $225
OR
Need help with your VA claim?
Get expert guidance and documentation from our licensed clinicians
Get Free ConsultationDr. Kishan Bhalani is a subject matter expert on VA disability claims documentation, with more than five years of focused work at the intersection of clinical m…
Dr. Kishan Bhalani is a subject matter expert on VA disability claims documentation, with more than five years of focused work at the intersection of clinical m…
Originally published May 2, 2026 • Last updated May 3, 2026
