Who Should Write Your VA Nexus Letter? A Clinician's Specialty-by-Specialty Guide (2026)

- 1.Why this question decides claims
- 2.Quick Answer: Which Specialist for Which Condition.
- 3.The Diagnosis vs. The Nexus: Two Different Medical Questions
- 4.Why the Provider You Choose Decides Your VA Claim
- 5.How the VA Weighs Medical Opinions: The M21-1 Probative Value Framework
- 6.Who Can Write a VA Nexus Letter? Eligibility Rules
- 7.Nexus Letter by Specialty: Provider-by-Provider Breakdown
- 8.When Internal Medicine Is the Right Writer (Even for "Specialty" Conditions)
- 9.Conditions Where Subspecialists Are Typically Considered
- 10.4 Common Provider-Selection Patterns We Observe
- 11.A 4-Question Educational Framework
- 12.Bottom Line: Match the Writer to the Question
- 13.How Military Disability Nexus Approaches Provider Selection
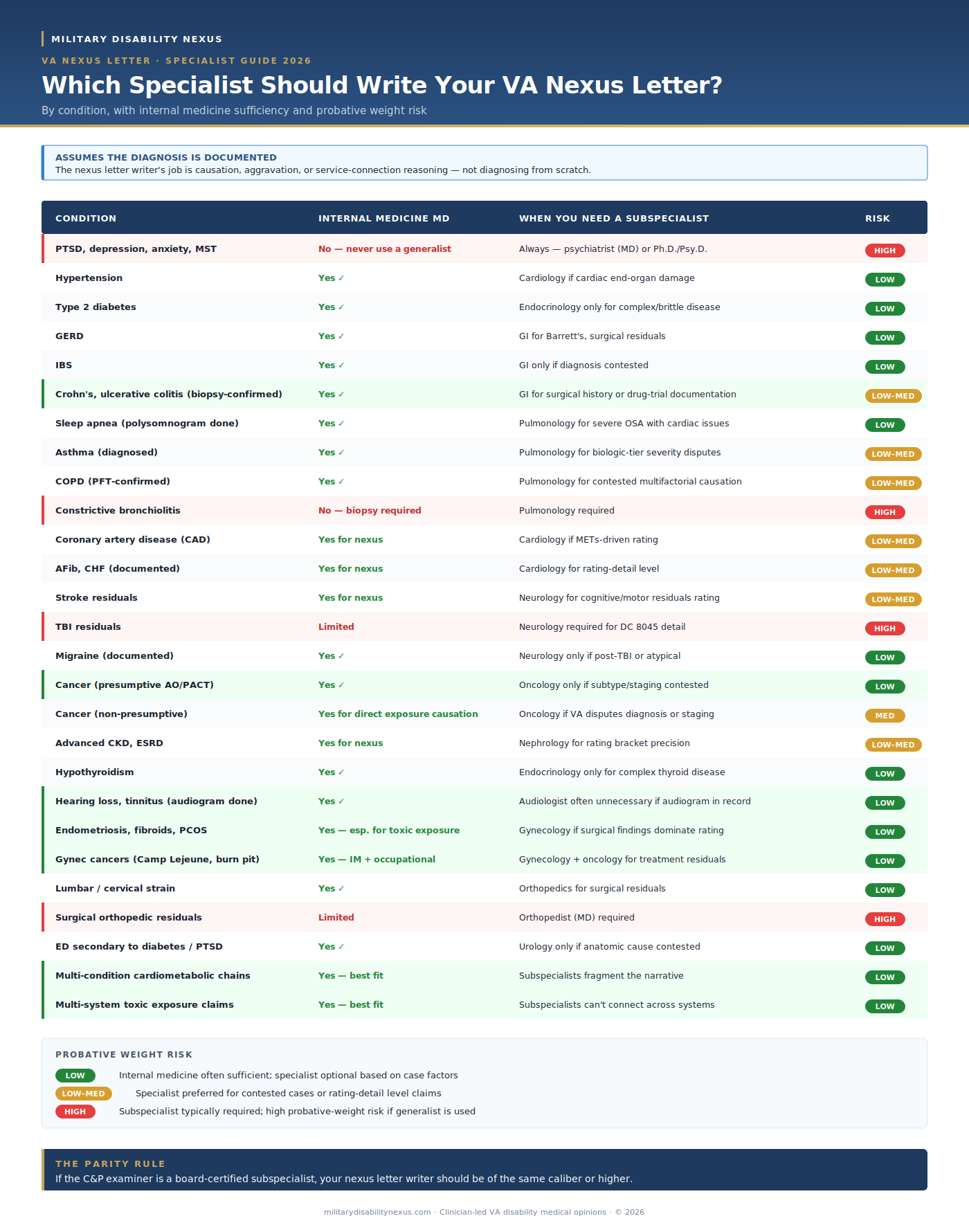
QUICK ANSWER:In our clinical experience, the VA generally gives meaningful weight to nexus letters when the writer's competence aligns with the medical question being asked. For mental health claims, the writer is typically a psychiatrist or Ph.D./Psy.D. psychologist. For many physical conditions where a diagnosis is already documented — including hypertension, diabetes, GERD, IBS, Crohn's, hearing loss, sleep apnea, and gynecologic conditions involving toxic exposure — a board-certified internal medicine MD may be well-positioned to write the nexus letter, particularly for multi-system or exposure-driven claims. Subspecialists are typically considered for cases where the diagnosis is contested, where surgical findings drive the rating, or where a board-certified specialist C&P opinion is in the record. Specific outcomes depend on case facts.
Why this question decides claims
Most veterans who reach out to us have already been denied at least once. When we walk back through their packet, the same pattern shows up over and over: the diagnosis was real, the in-service event was documented, and the nexus letter said all the right things - but it was written by a provider whose specialty didn't match the condition. The VA rater read it, gave it minimal probative weight, and the claim died on a technicality almost no veteran sees coming.
This article exists because the question of who writes your nexus letter matters as much as what the letter says. The VA's own M21-1 Adjudication Procedures Manual lists the provider's "qualifications to include his/her expertise/specialty, and experience" as the first factor in evaluating probative value. Specialty isn't a nice-to-have. It's the first thing the rater looks at.
We'll walk through every type of provider a veteran might use, what the VA does with each, which conditions each one is best suited for, and most importantly - when an Internal Medicine (MD) is the right call versus when a subspecialist is required.
Quick Answer: Which Specialist for Which Condition.
This table assumes the diagnosis is already documented in the record (audiogram done, colonoscopy done, biopsy done, imaging done, etc.). What you're hiring the nexus letter writer to do is explain causation, aggravation, or service connection — not to diagnose from scratch. Match your condition to the recommended specialty before you pay for any nexus letter.
Bottom-line rule: A board-certified internal medicine physician can write the nexus opinion on the vast majority of physical-medicine claims once a diagnosis is in the record. Subspecialists are essential when (1) the diagnosis is contested, (2) surgical findings dominate the rating, (3) the C&P examiner is a specialist whose negative opinion needs to be rebutted at parity, or (4) the specialty manages a unique rating scale (DC 8045 TBI, METs-based cardiac codes). For mental health, never use anyone but a psychiatrist or Ph.D./Psy.D. psychologist.
The Diagnosis vs. The Nexus: Two Different Medical Questions
This is the core insight that resolves most of the confusion about who should write a nexus letter.
Diagnosing a condition and writing a nexus opinion are two different medical exercises:
The diagnosis answers: Does this veteran have Crohn's disease? or Does this veteran have Hearing Loss? This may require a gastroenterologist's colonoscopy and biopsy, or an audiologist's audiogram.
The nexus opinion answers: Is this Crohn's disease at least as likely as not caused by, aggravated by, or secondary to military service? This is a causation and exposure-medicine question, and it's a core internal medicine competency.
Once the gastroenterologist has done the colonoscopy and signed the biopsy report, an internal medicine MD reading the chart, the STRs, the toxic exposure history, the post-service trajectory, and the published mechanism literature is fully qualified and often better qualified to write the nexus opinion. The gastroenterologist treats the Crohn's; the internist explains its origin.
The same logic holds across most conditions:
The audiologist documents the threshold shift on the audiogram. The internist writes the nexus opinion connecting it to MOS-related noise exposure.
The gynecologist does the laparoscopic staging of endometriosis. The internist writes the nexus opinion connecting it to TCE/PCE exposure at Camp Lejeune.
The cardiologist does the catheterization and confirms CAD. The internist writes the nexus opinion connecting it to PTSD-driven sympathetic activation and metabolic syndrome.
THE EXCEPTION THAT PROVES THE RULE:Mental health is different. The diagnosis is the nexus question - there's no separate biopsy or imaging that anchors the diagnosis. The diagnostic interview, mental status exam, and DSM-5 criteria application are all done by the same psychiatrist or psychologist who would write the nexus opinion. That's why the rule for mental health is absolute: always a psychiatrist or Ph.D./Psy.D. psychologist.
Why the Provider You Choose Decides Your VA Claim
Most veterans who reach out to us have already been denied at least once. When we walk back through their packet, the patterns split into two common failure modes:
The wrong-credential failure: a chiropractor wrote the PTSD letter, a family doctor wrote the constrictive bronchiolitis letter, an LCSW signed the formal nexus opinion. The diagnosis-vs-nexus framework was violated and the letter got minimal weight.
The over-specialization failure: a veteran spent thousands of dollars on three or four separate subspecialist letters when one internal medicine MD could have written a coordinated multi-condition opinion, often more effectively. The probative weight of disconnected letters is lower than the probative weight of one cohesive narrative.
The VA's M21-1 manual lists the provider's "qualifications to include his/her expertise/specialty, and experience" as the first factor in evaluating probative value. But "expertise" doesn't mean "narrowest possible subspecialty." It means competency in the medical question being asked.
The cost of getting this wrong: A poorly matched nexus letter costs $5000–$2,500, gets minimal weight, and the claim still requires re-filing. Equally costly: paying for four subspecialist letters at $2,500 each when one internal-medicine-led IMO at $1,500 would have been clinically stronger because it could connect the chain.
How the VA Weighs Medical Opinions: The M21-1 Probative Value Framework
When two medical opinions disagree - say, a positive nexus letter from your provider and a negative C&P opinion - the rater applies a five-factor probative-weight analysis from M21-1:
The provider's qualifications — specialty, board certification, experience, and demonstrated competence in the medical question at issue.
The provider's knowledge of the relevant history — did they review the C-file, STRs, and post-service records?
The context — treatment relationship, IME, or claim-substantiation.
The reasoning employed — clinical observation, testing, peer-reviewed literature, or conjecture.
The degree of specificity and certainty.
Notice that factor 1 is "qualifications," not "narrowest possible subspecialty." A board-certified internist writing about Crohn's is qualified - internal medicine residency includes gastroenterology rotations and tested competency in IBD pathophysiology. The factor that often matters more than narrow specialty is the depth and quality of the reasoning (factor 4) and that's where the right writer beats the wrong subspecialist.
What this means for you: A nexus letter from a chiropractor about a mental health condition fails factor 1 immediately. A nexus letter from a board-certified internist about Crohn's disease - once the diagnosis is documented and the rationale is anchored in stress-mechanism literature and toxic-exposure data - holds up against a generalist subspecialty letter that didn't engage the mechanism question.
Who Can Write a VA Nexus Letter? Eligibility Rules
The VA accepts nexus letters from:
Medical Doctors (MD) — fully accepted across all conditions
Doctors of Osteopathy (DO) — equivalent weight to MDs
Nurse Practitioners (NP) — accepted, weight tied to scope and clinical experience
Physician Assistants (PA-C) — accepted, weight tied to scope and clinical experience
Doctorate-level Psychologists (Ph.D. or Psy.D.) — accepted for mental health, equal weight to psychiatrists
Chiropractors — accepted for musculoskeletal opinions within scope only
Audiologists — accepted for hearing loss and tinnitus
The VA generally does NOT accept nexus letters from:
Licensed Clinical Social Workers (LCSWs) — collateral evidence only
Master's-level therapists (LPCs, MFTs) — collateral evidence only
Acupuncturists, naturopaths, herbalists, massage therapists, wellness coaches
Key takeaway: Eligibility is necessary but not sufficient. The probative weight depends on the match between the writer's competence and the medical question being asked - not on the number of years of post-residency subspecialty fellowship.
Nexus Letter by Specialty: Provider-by-Provider Breakdown
Reminder: The following sections describe general patterns we observe in VA claims work, based on our clinical team's experience. They are educational observations, not recommendations for any specific claim. Pricing ranges are general references reflecting publicly available market information; individual provider fees vary widely.
Internal Medicine MD: The Strongest Single Writer for Most VA Claims
May be considered for: Hypertension, diabetes (Type 1 and 2), GERD, IBS, Crohn's, ulcerative colitis, sleep apnea, CKD, stable CAD, hypothyroidism, hearing loss with documented audiogram, gynecologic conditions involving toxic exposure, multi-system toxic-exposure claims, multi-condition cardiometabolic chains.
Generally not the typical choice for: Mental health (psychiatrist or Ph.D./Psy.D. psychologist typically considered), surgical orthopedic residuals where operative findings drive the rating, TBI rating-detail under DC 8045.
General probative weight: May be substantial when the medical question aligns with internal medicine competency.
Typical cost in 2026: $1,000–$1,800 (single condition); $1,800–$3,500 (multi-condition coordinated IMO).
A board-certified internal medicine physician completes three years of residency covering cardiology, pulmonology, endocrinology, nephrology, gastroenterology, rheumatology, infectious disease, hematology, and oncology - with full diagnostic and management competency tested in each. That breadth is exactly what most VA nexus questions require, because most claims either span multiple systems or hinge on an exposure-medicine causation argument that an internist is trained to construct.
Why internal medicine works for the most common VA conditions:
Hypertension, diabetes, hyperlipidemia, metabolic syndrome: daily internal medicine.
GERD, IBS, Crohn's disease, ulcerative colitis (biopsy-confirmed): once the gastroenterologist has done the diagnostic workup, the nexus opinion (stress-mechanism, exposure-driven, secondary connection) is exposure-medicine reasoning, which internists do better than most narrow GI subspecialists.
Hearing loss and tinnitus: once the audiogram is done, the nexus question is occupational-exposure causation. An internist with occupational/exposure-medicine framing handles this competently.
Sleep apnea with polysomnogram: internist-territory nexus opinion on causation and aggravation.
Asthma, COPD, routine pulmonary disease: once PFTs are done.
Chronic kidney disease: Internal medicine until late-stage transplant referral.
Stable cardiac disease: diagnosed and co-managed by internists.
Hypothyroidism, anemia, vitamin deficiencies: routine internal medicine.
Gynecologic conditions in toxic-exposure cases: endometriosis, fibroids, and reproductive cancers in Camp Lejeune or burn-pit-exposed veterans are exposure-medicine claims as much as gynecologic claims. Internal medicine and occupational medicine are typically better positioned to write the causation opinion than a routine OB-GYN, who treats the disease but doesn't typically write toxic-exposure causation analyses.
Multi-condition cardiometabolic chains (PTSD → metabolic syndrome → hypertension → diabetes → CAD → CKD): an internist can write the entire chain in one cohesive narrative. This is a structural advantage over subspecialty letters that can each only address one link.
Cost-efficiency advantage: For a Vietnam-era veteran filing diabetes plus hypertension plus CAD plus diabetic neuropathy plus CKD, one internal-medicine-led IMO can address all five conditions in a single coordinated opinion. Five separate subspecialist letters would cost three to four times as much, would each have to cross-reference the others, and would lack the unifying mechanism narrative the rater can follow.
Bottom line: If your claim involves any combination of cardiometabolic, GI, endocrine, routine pulmonary, hearing, or toxic-exposure conditions — start with internal medicine. Subspecialists become important when the diagnosis itself is contested, when the rating turns on subspecialty-specific testing (METs, EMG, biopsy interpretation, surgical findings), or when a board-certified specialist C&P needs to be rebutted at credential parity.
Family Medicine MD: Comparable Breadth, Slightly Less Depth
Best for: Initial filings on routine adult conditions when there's a long-standing patient relationship.
Avoid for: Appeals after denial, complex secondary chains, contested claims.
General probative weight: May be considered for routine claims; weight on contested matters depends on case factors.
Typical cost in 2026: $800–$1,500.
Family medicine covers internal medicine plus pediatrics, obstetrics, and minor surgery. For VA claims, this typically translates to slightly less depth on the adult internal medicine pathophysiology that anchors strong nexus reasoning. Family medicine MDs can write competent letters on routine adult conditions when they're willing to do the literature work, but they're less commonly experienced in writing the kind of mechanism-anchored, citation-supported opinion that holds up on appeal.
Cardiologist: For Rating-Detail Cardiac Cases
Best for: Rating-detail cases where METs limitation, surgical history, or device-driven rating dominates. CAD with stenting/MI history, AFib with rhythm-strip documentation, CHF with serial echocardiograms, cardiomyopathy classification, aortic disease.
Avoid for: Routine nexus questions where the cardiac diagnosis is established and the rating isn't METs-driven (internist suffices).
General probative weight: May be substantial for rating-detail cardiac claims.
Typical cost in 2026: $1,800–$3,000.
A cardiologist's specialty weight matters most when the rating turns on METs limitation testing under DC 7005, DC 7007, or similar codes that require cardiologist measurement and interpretation. For routine nexus opinions on documented cardiac conditions — particularly Agent Orange ischemic heart disease where the presumption is the legal mechanism — an internist is typically sufficient.
Pulmonologist: For Diagnostic Edge Cases and Severe Disease
Best for: Constrictive bronchiolitis (often missed on standard PFTs, biopsy-required), severe persistent asthma on biologics, pulmonary fibrosis, sarcoidosis, complex sleep apnea with cardiac complications.
Avoid for: Routine asthma, COPD, sleep apnea (internist suffices once the diagnosis is documented).
General probative weight: May be substantial for complex respiratory claims.
Typical cost in 2026: $1,800–$3,000.
A pulmonologist is essential when the diagnosis itself is contested or the diagnostic workup requires biopsy interpretation. Constrictive bronchiolitis in burn-pit-exposed veterans is the clearest example. For routine asthma, COPD, or sleep apnea where the diagnosis is established, an internist is typically the better cost-quality balance.
Endocrinologist: For Diagnostic Complexity Only
May be considered for: Brittle Type 2 diabetes with complex management, pituitary disorders, Cushing's, Addison's, complex thyroid disease where diagnosis is contested.
Less commonly necessary for: Routine Type 2 diabetes, routine hypothyroidism (within internal medicine scope).
General probative weight: May be substantial for complex endocrine claims.
Typical cost in 2026: $1,800–$2,800.
For routine Type 2 diabetes - the most common endocrine claim - an internist handles the nexus opinion as well as or better than a subspecialty endocrinologist. Endocrinology weight matters when the diagnosis is unusual or the treatment course is genuinely complex.
Nephrologist: For Advanced Disease Rating Detail
May be considered for: ESRD, dialysis dependence, glomerular disease classification, transplant evaluation, rating bracket precision at advanced stages.
Less commonly necessary for: CKD stages 1–3, routine nexus opinions where the diagnosis is established.
General probative weight: May be substantial for advanced kidney disease rating detail.
Typical cost in 2026: $1,800–$2,800.
The VA rates kidney disease under § 4.115a, with rating brackets driven by GFR and dialysis status. For rating-detail precision at advanced stages, a nephrologist's documentation matters. For nexus opinions on documented CKD - particularly secondary to service-connected diabetes or hypertension - an internist is fully competent.
Gastroenterologist: For Diagnostic Workup, Not Always for Nexus
May be considered for: Cases where the diagnosis is contested, surgical history is at issue, drug-trial documentation matters for rating, or biopsy interpretation drives the claim.
Less commonly necessary for: Routine nexus opinions on already-diagnosed Crohn's, UC, IBS, GERD.
General probative weight: May be substantial when diagnostic questions are contested.
Typical cost in 2026: $1,800–$2,800.
This is one of the most commonly over-specified specialty selections. A gastroenterologist does the colonoscopy and signs the biopsy. Once that diagnosis is in the record, the nexus opinion -connecting the IBD to PTSD, stress mechanism, toxic exposure, or service-onset - is exposure-medicine reasoning that an internist often writes more effectively than a GI subspecialist whose focus is treatment, not causation. Gastroenterology weight becomes important when the VA contests the diagnosis itself or when surgical residuals dominate the rating.
Neurologist: For TBI Rating-Detail and Neurodegenerative Disease
May be considered for: TBI residuals at DC 8045 rating-detail level (cognitive, behavioral, somatic domains), MS, ALS, Parkinson's, complex post-traumatic migraine, peripheral neuropathy when EMG/NCS interpretation is decisive.
Less commonly necessary for: Routine migraine, peripheral neuropathy secondary to documented diabetes, routine stroke nexus once residuals are documented.
General probative weight: May be substantial for neurological rating detail.
Typical cost in 2026: $1,800–$3,000.
Neurology weight is essential when the rating mechanism itself is neurology-specific - TBI domains being the clearest example. For routine migraine secondary to TBI, or peripheral neuropathy secondary to service-connected diabetes, an internist handles the nexus competently.
Oncologist: For Contested Cancer Cases
May be considered for: Non-presumptive cancers where direct exposure causation is at issue, contested staging or subtype, treatment residuals (chemo-induced neuropathy, radiation pneumonitis, treatment-induced cardiomyopathy), DIC/survivor cause-of-death claims.
Less commonly necessary for: Straightforward presumptive cancer claims under Agent Orange or PACT Act.
General probative weight: May be substantial for contested cancer claims.
Typical cost in 2026: $2,000–$3,500.
For presumptive cancer claims, the legal presumption is the mechanism - the writer's job is to confirm the diagnosis and document the qualifying service. An internist or family medicine physician handles this. Oncology weight matters most when the cancer is non-presumptive and direct exposure causation must be argued, when subtype classification is disputed, or when treatment residuals warrant separately rated secondary conditions.
Psychiatrist (MD) and Psychologist (Ph.D./Psy.D.): For All Mental Health Claims
Typically considered for: PTSD, MDD, GAD, panic disorder, MST claims, bipolar disorder, mental health secondary to chronic pain, substance use disorder secondary to PTSD.
General probative weight: Typically substantial for mental health claims.
Typical cost in 2026: $1,500–$3,000.
This is the area where the diagnosis-vs-nexus framework collapses into a single question that only a mental health specialist can answer. Mental health diagnosis is interview-based, mental-status-exam-based, and DSM-5-criteria-based — there's no separate biopsy or imaging that anchors the diagnosis, so the same provider who would diagnose is the one who must write the nexus opinion.
Equal-weight writers:
Board-certified psychiatrist (ABPN) — particularly valuable when medication is part of the claim, when differential diagnosis is contested, or when comorbid medical conditions complicate the picture.
Doctorate-level clinical psychologist (Ph.D. or Psy.D.) — equally weighted for diagnosis, course, and rating-relevant functional impairment under § 4.130. Often the more affordable option.
⚠️ CRITICAL WARNING:
An internist or family medicine MD should not be writing primary mental health nexus letters. This is the most common avoidable error we see.
Orthopedist: For Surgical Cases Only
May be considered for: Surgical residuals, hardware complications, total joint replacements, severe DJD with surgical recommendations, imaging-driven rating where operative findings are at issue.
Less commonly necessary for: Routine lumbar or cervical strain, mechanical back pain, soft-tissue musculoskeletal conditions.
General probative weight: May be substantial for surgical orthopedic claims.
Typical cost in 2026: $2,000–$3,000.
Orthopedic surgeon weight becomes essential when operative findings, hardware, or surgical history drive the rating. For non-surgical musculoskeletal conditions, the internal medicine + chiropractor (in scope) combination typically handles these claims at lower cost and equal weight.
Chiropractor: Narrow but Legitimate for Spine Claims
May be considered for: Cervical and lumbar mechanical strain, spinal range-of-motion documentation, sacroiliac dysfunction, post-traumatic spinal injury without surgery.
Generally outside scope: Conditions outside the musculoskeletal system, including post-surgical spine, hardware, mental health, respiratory, cardiac, GI, or systemic conditions.
General probative weight: May be considered within scope; typically lower outside scope.
Typical cost in 2026: $400–$1,000.
The VA accepts chiropractor opinions, but the weight depends entirely on whether the opinion stays within scope of practice.
Audiologist: Helpful but Often Unnecessary
May be considered for: Hearing loss and tinnitus claims where audiogram interpretation is contested or adds value.
General probative weight: Generally considered authoritative within auditory scope.
Typical cost in 2026: $500–$1,200.
Once the audiogram is in the record showing the noise-induced threshold pattern, the nexus opinion is occupational-exposure causation reasoning which an internist with occupational-medicine framing handles competently. An audiologist's letter can add weight if the audiogram interpretation is contested, but for most hearing loss and tinnitus claims an internal medicine nexus opinion citing the audiogram is sufficient.
Ophthalmologist (MD) and Optometrist (OD): For Eye Conditions
Ophthalmologist may be considered for: Surgical eye conditions, advanced glaucoma, post-traumatic eye injury with surgical residuals.
Optometrist may be considered for: Routine refractive issues, mild dry eye, diabetic retinopathy screening.
General probative weight: Ophthalmology may carry more weight for advanced/surgical disease.
Typical cost in 2026: $1,000–$2,500.
For nexus opinions on diabetic retinopathy or other diabetes-secondary eye conditions, an internist who can connect the eye finding to the documented diabetes writes a competent nexus letter once the ophthalmology imaging is in the record.
Gynecologist: For Surgical and Diagnostic Workup
May be considered for: Surgical staging documentation (laparoscopic findings in endometriosis), gynecologic cancer treatment, complex pelvic surgical residuals where surgical findings dominate the rating.
For toxic-exposure-driven gynecologic conditions: Internal medicine or occupational-medicine framing may also be considered, since the central question is often exposure causation rather than gynecologic treatment.
General probative weight: May be substantial for surgical residual documentation.
Typical cost in 2026: $1,800–$2,800.
This is another area commonly over-specified. A gynecologist treats endometriosis, fibroids, and gynecologic cancers — but writing a nexus opinion connecting these conditions to TCE/PCE exposure at Camp Lejeune, or to burn-pit exposure, is toxic-exposure medicine reasoning, not routine gynecology. An internist or occupational medicine physician with gynec disease familiarity often writes a more compelling toxic-exposure causation opinion than a routine OB-GYN whose practice focuses on treatment, not causation analysis.
Gynecology weight is most useful when surgical findings (laparoscopic endometriosis staging, fibroid imaging, surgical pathology) need to be incorporated into the rating documentation — not necessarily for the causation opinion itself.
Physician Assistant (PA-C): Capable, Cost-Effective for Routine
May be considered for: Routine claims where the PA-C has clear specialty alignment with the condition.
Less common for: Appeals after a specialist's negative C&P, contested claims with conflicting specialist opinions.
General probative weight: May depend on specialty alignment.
Typical cost in 2026: $500–$1,500.
A PA-C in a cardiology practice writing about hypertension carries reasonable weight; a PA-C in dermatology writing about hypertension does not.
Nurse Practitioner (NP / DNP): Same Profile as PA
May be considered for: Routine claims, particularly with specialty NPs (PMHNP for mental health, AGNP for adult medicine).
Less common for: Appeals after a specialist's negative C&P.
General probative weight: May depend on specialty alignment
Typical cost in 2026: $400–$1000.
A psychiatric NP (PMHNP) writing about PTSD carries reasonable weight; a family-practice NP writing about Crohn's disease does not.
When Internal Medicine Is the Right Writer (Even for "Specialty" Conditions)
Most veterans assume specialty-named conditions require specialty writers. They usually don't, once the diagnosis is documented. Internal medicine is the right writer when:
The diagnosis is established in the record by the appropriate diagnostic specialist (audiogram done, biopsy done, imaging done, polysomnogram done).
The medical question is causation, aggravation, or secondary connection rather than diagnostic clarification.
Toxic exposure medicine is part of the claim - Camp Lejeune, Agent Orange, burn pits, K2 — internal and occupational medicine handle these claims at higher quality than narrow subspecialties whose practice doesn't routinely engage exposure causation.
Multi-system or multi-condition chains exist — internal medicine can connect them in one cohesive opinion.
The veteran is filing on a budget and needs the strongest writer per dollar — internal medicine is typically the best cost-quality ratio for the largest range of conditions.
Specific conditions where internal medicine is often the right writer despite the "specialty" appearance:
Hearing loss and tinnitus (audiogram in record)
Crohn's disease and ulcerative colitis (biopsy-confirmed)
Asthma and COPD (PFT-confirmed)
Sleep apnea (polysomnogram-confirmed)
Diabetic retinopathy (ophthalmology imaging in record)
Endometriosis, fibroids, PCOS in toxic-exposure cases
Reproductive cancers in Camp Lejeune or burn-pit veterans
Established cardiac disease where rating isn't METs-driven
Stroke residuals where the nexus is the question, not the rating detail
Peripheral neuropathy secondary to diabetes
Cancer claims under presumptive frameworks
Multi-condition cardiometabolic chains (the highest-value internist scenario)
Conditions Where Subspecialists Are Typically Considered
In our experience, subspecialist input is typically considered for:
Mental health claims — psychiatrist (MD) or Ph.D./Psy.D. psychologist
TBI residuals at rating-detail level (DC 8045) — neurology
Constrictive bronchiolitis — pulmonology
METs-driven cardiac rating — cardiology
ESRD and advanced kidney disease rating — nephrology
Surgical orthopedic residuals where operative findings drive rating — orthopedist (MD)
ALS, MS, Parkinson's progression rating — neurology
Cancer claims with contested diagnosis or staging — oncology
Severe IBD with surgical history at issue — gastroenterology
Surgical gynecologic residuals — gynecology
General consideration: When the C&P examiner is a board-certified subspecialist who has issued a negative opinion, considering a rebuttal writer at credential parity may be relevant. This is sometimes called the "parity" consideration.
4 Common Provider-Selection Patterns We Observe
Across the claims we review, certain patterns appear regularly. These are general observations from our clinical team's experience, not assessments of any specific provider or claim.
Pattern #1: Generalist Providers Writing Mental Health Letters
In our experience, mental health is one area where the diagnostic and nexus-writing competencies are typically inseparable. Both generally require psychiatric or psychologic specialty training. We sometimes see family medicine providers asked to anchor PTSD claims; in our observation, the probative weight assigned by the VA in such cases may be lower than when mental health specialty input is provided.
Pattern #2: VA Treating Providers and Nexus Letter Constraints
Veterans we work with sometimes report institutional constraints when requesting nexus letters from VA-employed providers — including time limitations, internal policies, and concerns about scope. Some VA providers do write nexus letters; others may decline. We encourage veterans to consult with a VA-accredited representative about whether a treating-provider letter, an independent medical opinion, or both are appropriate for their specific situation.
Pattern #3: Multiple Disconnected Subspecialist Letters
When veterans obtain several separate subspecialist letters for related conditions, the resulting evidence package may be more expensive without necessarily being clinically stronger than a single coordinated opinion. In our experience, the cohesive mechanism narrative of a single coordinated IMO may carry weight that fragmented letters do not, particularly for multi-condition cardiometabolic, exposure-driven, or PTSD-secondary chains.
Pattern #4: The "Specialty Name Equals Specialty Writer Required" Assumption
Conditions named after a specialty (such as "Crohn's disease" or "tinnitus") sometimes lead veterans to assume only that specialty can write the nexus letter. In our clinical experience, once the diagnostic workup is complete, the nexus question often becomes causation analysis — which may fall within internal medicine's scope.
A 4-Question Educational Framework
Important: The framework below is general educational guidance. Specific provider selection for any individual claim involves judgment about factors that may not be addressed here. We strongly encourage veterans to consult with a VA-accredited representative before making decisions about their claim..
Question 1: Is the diagnosis itself documented and uncontested?
If yes, the nexus question is generally causation/aggravation reasoning, which may fall within internal medicine scope. If no, a relevant subspecialist may be considered to anchor the diagnosis first.
Question 2: What does the rating turn on?
If the rating turns on subspecialty-specific testing (METs, EMG, biopsy interpretation, surgical findings, DC 8045 domain assessment), that subspecialist's input may be particularly relevant. If the rating turns on standard clinical documentation, internal medicine may often be sufficient.
Question 3: Has the VA examiner already issued a contrary opinion, and what is their specialty?
Considering credential parity for rebuttals may be relevant. A negative opinion from a board-certified pulmonologist may be most effectively addressed by a pulmonologist rebuttal.
Question 4: How many conditions are you filing on, and do they share a mechanistic root?
Multi-condition cardiometabolic, exposure, or PTSD-driven chains may favor a single internal-medicine-led IMO. Single-system contested-diagnosis cases may favor a subspecialist.
FAQ
Can any doctor write a VA nexus letter?
Generally, any licensed healthcare provider competent in the medical question being asked may write a VA nexus letter. The VA's M21-1 manual considers the provider's qualifications among multiple factors when evaluating probative weight. A board-certified internist may be well-positioned to address many non-mental-health nexus questions once a diagnosis is documented, though specific outcomes depend on case facts. This is general educational information and not advice for any specific claim.
Does the VA give more weight to subspecialists than to internal medicine MDs?
Not automatically. The manual generally considers qualifications including expertise, specialty, and experience among multiple factors — not narrowest possible subspecialty alone. The depth of reasoning and engagement with the medical question may also be considered. Subspecialists may carry more weight when the rating or diagnosis depends on their unique competency. Outcomes vary by case.
Can my primary care internal medicine doctor write my VA nexus letter for Crohn's disease?
In our clinical experience, an internal medicine MD may be well-positioned to write a nexus opinion for Crohn's disease once the diagnosis has been confirmed by appropriate diagnostic workup. Internal medicine training generally covers IBD pathophysiology, and the nexus question is often about causation analysis rather than diagnosis. Whether this approach fits a specific claim depends on individual case factors, including any prior C&P opinions in the record.
Can an internist write a nexus letter for hearing loss and tinnitus?
An internal medicine MD with familiarity in occupational-exposure causation may write a competent nexus opinion when an audiogram is documented in the record. Many veterans we work with have found this approach effective, though an audiologist letter may add weight in cases where audiogram interpretation is contested or where the C&P opinion is from an audiologist.
Can an internist write a nexus letter for endometriosis or other gynecologic conditions?
In our experience, an internal medicine or occupational-medicine-trained physician may be well-positioned to write nexus opinions for gynecologic conditions in toxic-exposure cases (such as Camp Lejeune or burn pit claims), where the central medical question is exposure causation rather than gynecologic treatment. Gynecology specialty input is often most useful when surgical findings or treatment residuals drive the rating. Specific claim strategy varies by case.
Can a chiropractor write a nexus letter for VA disability?
The VA generally accepts chiropractor opinions for musculoskeletal claims within their scope of practice — such as cervical strain, lumbar strain, sacroiliac dysfunction, and mechanical spinal pain. For conditions outside the musculoskeletal system, chiropractor opinions are typically given less probative weight by the VA. Veterans should consult a VA-accredited representative about their specific situation.
Can a nurse practitioner write a VA nexus letter?
The VA generally accepts nurse practitioner nexus letters. The probative weight may depend on the NP's specialty alignment with the condition. A psychiatric NP writing about a mental health condition is typically considered differently than a family-practice NP writing about a complex specialty condition. Specific outcomes depend on the totality of the evidence in each case.
Should I ask my VA doctor to write my nexus letter?
VA-employed providers are generally permitted to write nexus letters, though some may decline due to institutional constraints. Veterans we work with report varied experiences with this approach. We encourage veterans to consult a VA-accredited representative about whether a treating-provider letter, an independent medical opinion, or both fit their specific situation.
What specialist should write my PTSD nexus letter?
Mental health claims, including PTSD, are generally best supported by opinions from psychiatrists (MD) or doctorate-level clinical psychologists (Ph.D. or Psy.D.). The diagnostic and nexus-writing competencies for mental health are typically inseparable. Veterans should discuss specific claim strategy with a VA-accredited representative.
Does a board-certified subspecialist guarantee my VA claim will be approved?
No. Probative weight is multifactorial — specialty, record review, rationale, literature citation, and correct legal standard all may be considered. A subspecialist letter that is not thoroughly reasoned may carry less weight than a well-reasoned internal medicine letter. Outcomes depend on the totality of the evidence.
Bottom Line: Match the Writer to the Question
In our clinical experience, the veterans who navigate provider selection most effectively often consider the writer-selection question alongside the medical content of the letter itself. Some general patterns we observe:
Mental health claims → psychiatrist or Ph.D./Psy.D. psychologist typically considered.
Documented physical conditions where the question is causation, aggravation, or secondary connection → internal medicine MD may be well-positioned, particularly for multi-condition or exposure-driven claims.
Subspecialist-considered claims (TBI rating-detail, METs cardiac, ESRD rating, surgical residuals, contested cancer, constrictive bronchiolitis) → appropriate subspecialist input.
Rebuttal at credential parity when a specialist C&P has issued a negative opinion.
These patterns are observations from our clinical experience, not guarantees of outcomes for any specific claim. Provider selection should be discussed with a VA-accredited representative.
How Military Disability Nexus Approaches Provider Selection
When we work on independent medical opinions, we begin with a structured clinical review that considers the writer-selection question. We do not apply a one-size-fits-all writer to every condition. For a multi-condition claim, we may engage an internal medicine physician for the cardiometabolic chain, the toxic-exposure analysis, and the secondary connection logic — and a psychiatrist for any mental health condition. The goal is to align each opinion with the specific medical question being asked.
Military Disability Nexus provides independent medical opinions for veterans pursuing VA disability claims. We do not represent veterans in claims preparation or adjudication; veterans seeking representation should work with a VA-accredited attorney, claims agent, or VSO representative.
⚠️ COMPREHENSIVE DISCLAIMER
Educational purpose only.This article reflects the general experience and perspective of the Military Disability Nexus clinical team. It is not medical advice, legal advice, or claims-preparation guidance for any specific veteran or claim. Outcomes for VA disability claims depend on case-specific facts, evidence, and applicable regulations.
Not legal representation.Military Disability Nexus provides independent medical opinions. We are not VA-accredited attorneys, claims agents, or Veterans Service Organization representatives. Under 38 CFR § 14.629, only VA-accredited representatives may provide claims-preparation services for compensation. Veterans seeking representation in VA disability claims should work with a VA-accredited attorney, claims agent, or VSO representative.
Information may change.The M21-1 Adjudication Procedures Manual is updated periodically; veterans and their representatives should consult the current authoritative version. VA presumptive lists, rating criteria, and other regulations are subject to change. Provider availability and pricing also change over time.
No guarantees.Provider selection considerations described in this article are based on patterns we observe in our work. They are not guarantees that any particular provider type will result in a favorable outcome for any specific claim. The probative weight assigned to any medical opinion is determined by the VA based on multiple factors, not solely on provider specialty.
Fee considerations.Veterans should be aware that fees for VA claims-related services are governed by 38 CFR § 14.636 and related regulations. We recommend flat-fee arrangements for medical opinions and encourage veterans to consult a VA-accredited representative about any fee arrangement that raises questions.
Authority for any specific claim.For specific guidance on a VA disability claim, veterans should consult with a VA-accredited attorney, claims agent, or VSO representative, and review the VA's M21-1 manual and applicable regulations directly..
CONTACT USHave Questions About a Medical Opinion for Your Claim?
Need help with your VA claim?
Get expert guidance and documentation from our licensed clinicians
Get Free ConsultationDr. Kishan Bhalani is a subject matter expert on VA disability claims documentation, with more than five years of focused work at the intersection of clinical m…
Dr. Kishan Bhalani is a subject matter expert on VA disability claims documentation, with more than five years of focused work at the intersection of clinical m…
Originally published April 26, 2026 • Last updated April 27, 2026
